Dear Editor,
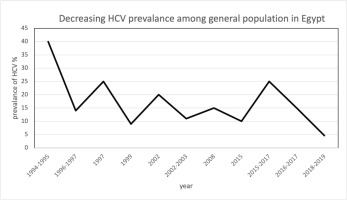
Hepatitis C Virus (HCV) has been a major health issue in Egypt for the past fifty years. It started in the 1960s when the government carried out mass treatment campaigns to eradicate Schistosomiasis among its population. Lack of sterilization and reuse of non-disposable needles led to the rapid spread of HCV1. The Ministry of Health started to address the epidemic in 2006 in a more comprehensive manner by establishing the National Committee for Viral Hepatitis in 2006, with the aim of eradicating HCV by 20302. The government was successful at locally manufacturing antivirals, thus drastically reducing treatment costs. Availability of treatment centers and lower-cost antivirals paved way for massive screening campaign in 2018. Within a year, every adult aged >18 years underwent screening, and those positive for HCV were mandated to get state-funded care4. Egypt treated over 2 million individuals since 2014, drastically reducing the HCV prevalence (Figure 1). In the 2018 screening, 4.6% of the previously untreated adults tested positive, making Egypt still one of the greatest HCV-burdened countries in the world5,6. The incidence of HCV infection in the Nile Delta, a high prevalence region, was approximately 6.1 people per 1000 in 2005, but declined to 2.4 per 1000 in 2010, and 0.37 per 1000 in 20187.
Despite the achievements, there is a need to invigorate the initiatives because of a number of challenges Egypt is facing. Major challenges include stigma, patients’ lack of knowledge, fear of discrimination, ignorance, and hesitancy to respond when asked about risky behavior. Stigma has been reported to reduce patients’ health seeking behavior and lessen their interaction with the medical system8. Additionally, Egypt’s conservative nature has hindered the use of needle-exchange facilities, a common preventive method for intravenous drug users in Europe9. The use of safety-engineered syringes as a prevention strategy may provide substantial population-level health gains10. Use of sharp-injury-protection syringes, recommended by the WHO, may reduce the incidence of needle-stick injuries among healthcare workers and patients10.
It is imperative to implement cost-effective programs to encourage people to adopt risk-reduction behaviors, address misunderstandings, and reinforce social support. It is important to make HCV and its eradication an explicit public health priority in Egypt. As initiated in Europe, establishing a Hepatitis Awareness Week would be greatly effective in Egypt. Health promotion strategies, including peer-to-peer counseling, could be tapped to clarify misconceptions and to strengthen social support for HCV patients. Young people can play a vital role in spreading awareness through national health campaigns. Local community members can be used as channels to provide information about the methods of transmission of HCV. They can also be trained to provide social and emotional support, especially in rural areas where prevalence is high and contradicting traditional beliefs remain influential. The use of information technology including online platforms, social media and hybrid educational approaches might be beneficial in providing information about HCV modes of transmission, drug safety, and prevention of IVDU to change public behavior. This approach will contribute to the removal of stigmatization of the affected groups, thus enabling them to benefit from opportunities for HCV testing, treatment, and prevention.